
(Photo Credit: Crucial Interventions)
According to the American Academy of Ophthalmology, roughly 24.4 million Americans aged 40 or older have cataracts (American Academy of Ophthalmology). Cataracts are typically defined as a condition in which the lens of the eye becomes clouded; thus reducing the person’s vision. Some common factors that are known to cause the loss of transparency to the eye lens can include aging, tobacco use, long exposure to sunlight and ultraviolet rays, certain medications, diabetes, hypertension, and a preexisting family history (Parker 86). The term, “cataract” derives from the Greek work for “waterfall” because prior to the 1700’s, people thought opaque material would somehow find a way to flow into the eye like a waterfall (Unite For Sight). Peter James, a historian, and Nick Thorpe, an archaeologist, made this statement about cataracts, “One of the most delicate parts of the body on which a surgeon can operate is the eye…yet ophthalmic surgery was one of the most advanced areas of medicine in the ancient world” (Pickover 36). We know that outpatient treatments for this eye condition do exist today, but procedures aimed to clear one’s vision after the formation of a cataract began more than 2,000 years ago (Parker 86). We are going to dive into the history and gradual development of cataract surgery in order to fully understand and appreciate how we got to the point of outpatient treatment and artificial lenses.

(Photo Credit: Medicine: The Definitive Illustrative History)
Needle couching was one of the most popular ways to treat a cataract. A Greek Philosopher explained in heavy detail the procedure in, De Medicina, a popular medical text at the time (Parker 86). The eye of the patient would be held open and a needle would pierce through the opaque lens. The surgeon would push the lens downward, leaving space for light to enter the eye. This method was, as we can imagine, extraordinarily painful, had a long recovery period, and left the patient without a focusing lens (Parker 86). Sometimes the physician would choose, instead, to slice the cataract up into tiny pieces and leave them to be absorbed by the body with time (Unite For Sight). This could cause fragments to lodge themselves into the jellylike structure of the eyeball and could cause a total loss of vision. Another treatment was to actually hit the eye when the cataract was ripe, meaning that it hardened and felt stiff to the touch. Hitting the eye’s surface was supposed to rupture the ligaments that held the lens onto the eye, and would allow the opaque lens to slide free (Parker 86). If the eye was hit too hard that could cause damage to the cornea and if the lens was not ripe, then hitting it would cause it to break into fragments (Parker 86).
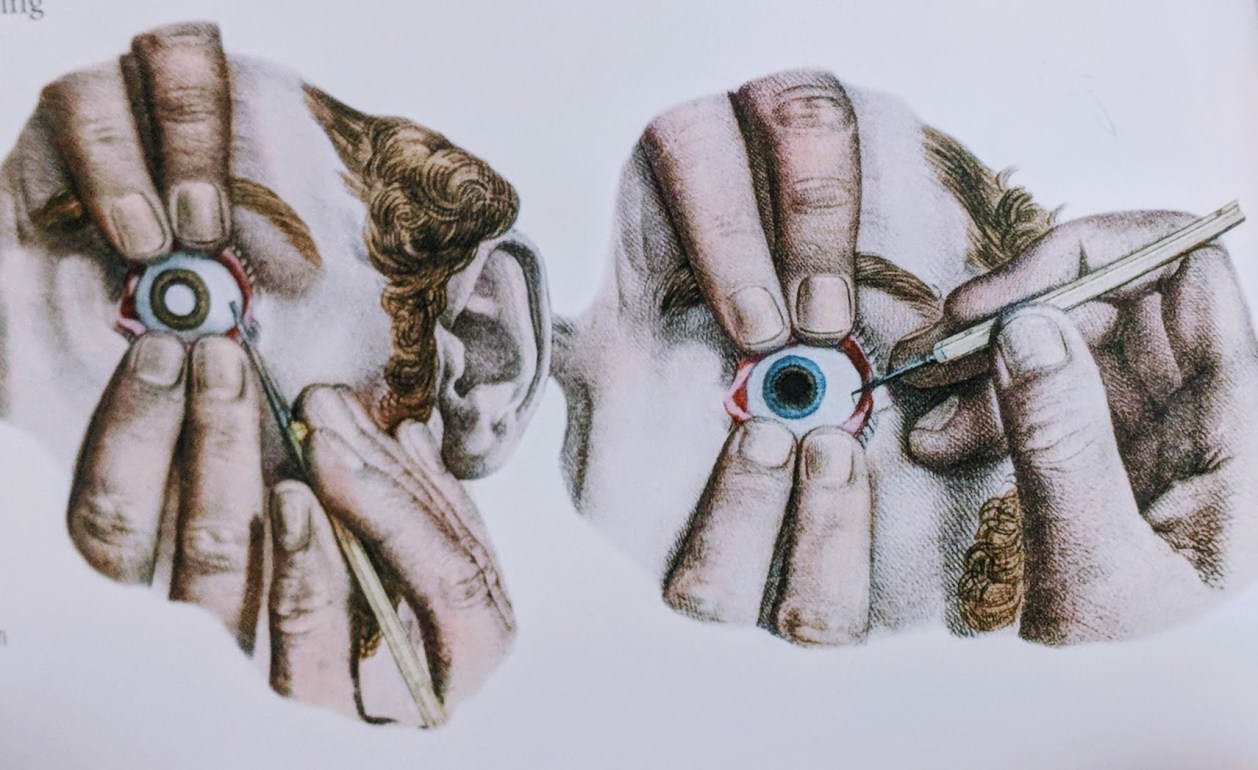
(Photo Credit: Medicine: The Definitive Illustrated History)
In 1748 the Frenchman, Jacques Daviel, developed a new surgical method. He would cut a c-shape into the eye and expand the opening with curved scissors. He would then insert a spatula and would free the lens from the rest of the eye. Using the spatula or a needle, Daviel would then pop the lens out of the incision. If the lens fell apart, a curette would retrieve the pieces and the eye would be bandaged (Parker 86). The patient would be left immobilized for days-sometimes even weeks after undergoing the treatment. Another major advancement would not come until 1967 when the US Ophthalmologist, Charles Kelman, developed phacoemulsification. A small incision would be made and an ultrasonic tip would then be placed inside the eye between the cornea and the lens (Parker 86). The tip would vibrate the lens and loosen it to the point where it could safely be sucked out of the eye. Harold Ridley helped make this procedure successful with the discovery of the artificial lens in the 1950’s. The lens was flexible enough that after the cataract was removed, the new one could be folded and inserted into the eye through the minor incision (Parker 86). Patients were no longer left without a focusing lens after the adjustment of their clouded vision! Cataract surgery serves millions of people every year worldwide. In fact, about 90% of people who undergo the surgery have improved vision afterwards (National Eye Institute). Although the earlier treatments have a way of making your skin crawl, they were advanced for their time. Seemingly barbaric methods like couching helped pave the way for safer and more effective practices.
(Photo Credit: Crucial Interventions)
(If that didn’t make you grateful for modern medicine, then I don’t know what will!)
Until Next Time
N.F.
Sources:
- American Academy of Ophthalmology. “Eye Health Statistics.” Accessed 17 October, 2018. https://www.aao.org/newroom/eye-health-statistics.
- Barnett, Richard. Crucial Interventions: An Illustrated Treatise on the Principles and Practice of Nineteenth Century Surgery. London: Thames and Hudson, 2015.
- National Eye Institute. “Facts About Cataracts.” Modified September 2015. Accessed 17 October, 2017. https://nei.nih.gov/health/cataract/cataract-facts.
- Parker, Steve. Medicine: The Definitive Illustrated History. New York: DK Publishing, 2016.
- Pickover, Clifford. The Medical Book. New York: Sterling Publishing, 2012.
- Unite For Sight. “Cataract Surgery: Across Time.” Accessed 17 October, 2018. http://www.uniteforsight.org/global-health-university/cataract-surgery.
This is a great post thaanks
LikeLike